Understanding ED and the Need for New Treatments
Erectile dysfunction (ED) is defined as the inability to achieve or maintain an erection sufficient for satisfactory sexual activity. This condition significantly impacts personal relationships, emotional well-being, and overall quality of life. ED becomes more prevalent with age, particularly among men over 40, though it can affect men of all ages.
The underlying causes of ED are diverse and often interconnected. Physical factors include poor blood circulation, cardiovascular disease, diabetes, obesity, hormonal imbalances, and nerve damage. Psychological contributors such as stress, anxiety, depression, and relationship difficulties also play significant roles. Lifestyle factors—including smoking, excessive alcohol consumption, sedentary habits, and poor diet—further increase ED risk.
Research Reference: Liu MC, Chang ML, Wang YC, et al. "Revisiting the Regenerative Therapeutic Advances Towards Erectile Dysfunction." Cells 2020, 9, 1250. DOI: 10.3390/cells9051250
Limitations of Conventional ED Treatments
While various surgical and non-surgical approaches have been developed to address ED, many conventional treatments have significant limitations:
PDE5 Inhibitors (Viagra, Cialis, Levitra)
These oral medications are effective for many men but can cause side effects including headaches, flushing, nasal congestion, and digestive issues. They require an intact nerve response system to work and cannot be used with certain heart medications.
Intracavernosal Injections
Injectable medications provide an alternative for men who don't respond to oral drugs, but they cause discomfort, have high discontinuation rates, and offer only short-term effects.
Surgical Interventions
Penile prostheses and other surgical options are typically reserved as last-resort treatments due to their invasiveness, high cost, and irreversibility.
These limitations have driven researchers to explore regenerative medicine approaches that aim to restore natural erectile function rather than simply treating symptoms.
Emerging Regenerative Therapies
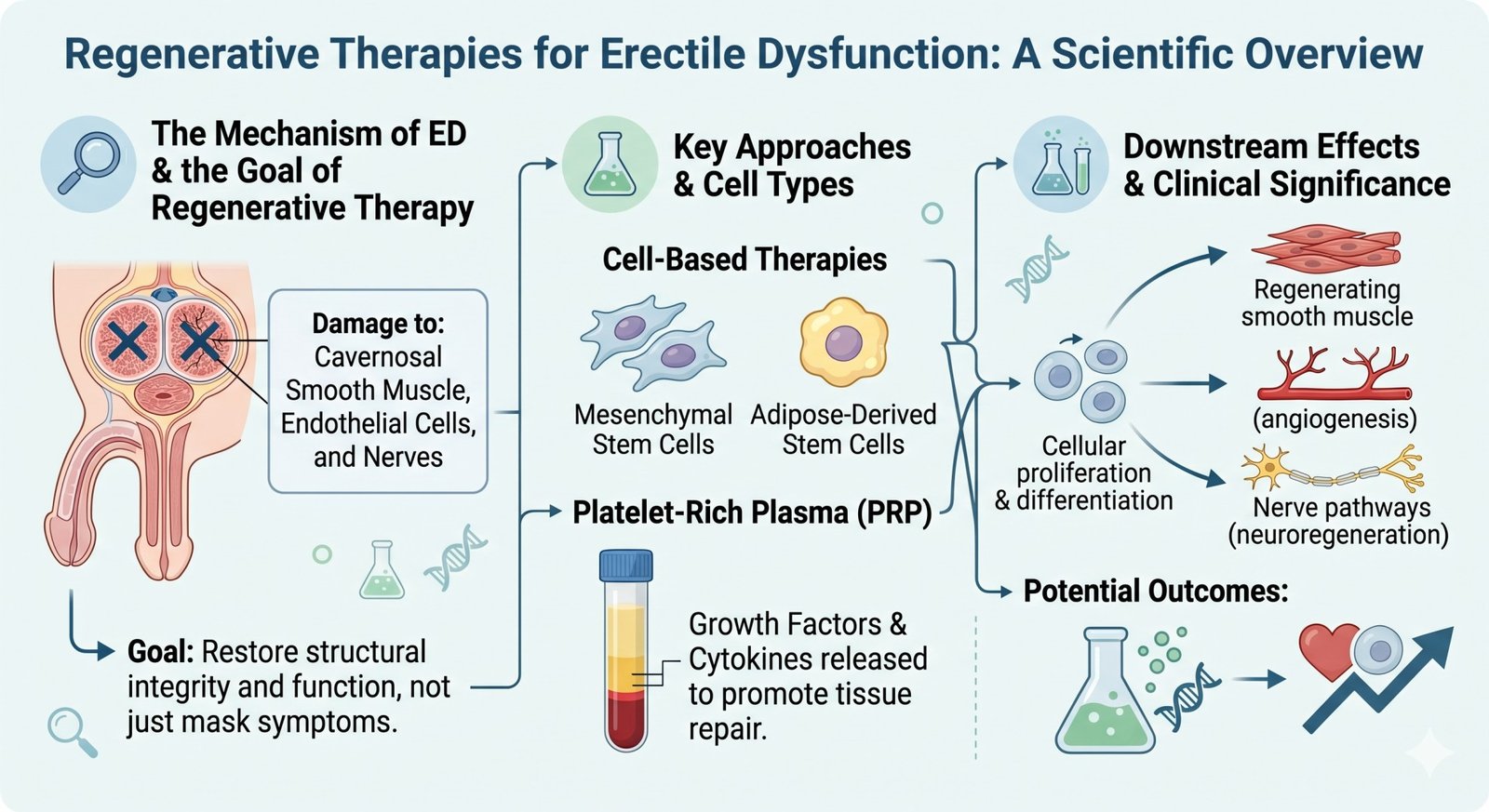
Regenerative medicine offers a fundamentally different approach to ED treatment by targeting the underlying tissue damage and dysfunction rather than temporarily overriding symptoms. The most promising regenerative therapies include:
Platelet-Rich Plasma (PRP)
Blood-derived PRP contains concentrated growth factors that promote tissue regeneration, angiogenesis, nerve repair, and collagen synthesis in penile tissues.
Stem Cell Therapy
Various stem cell types including adipose-derived, bone marrow-derived, and induced pluripotent stem cells show promise in regenerating damaged cavernous nerve tissue.
Low-Intensity Shockwave
LI-ESWT triggers revascularization, releases angiogenic factors, and promotes neovascularization to improve blood flow in injured penile tissue.
Combined Approaches
Research shows that combining therapies—such as stem cells with PRP or shockwave therapy—may produce synergistic effects for enhanced outcomes.
Platelet-Rich Plasma (PRP) Therapy
Platelet-rich plasma is derived from a patient's own blood through a centrifugation process that concentrates platelets and their associated growth factors. When activated and injected into penile tissue, PRP releases a cascade of regenerative biomaterials that promote healing and tissue restoration.
Key Growth Factors in PRP
PRP contains numerous growth factors, chemokines, and angiogenic factors that work together to support tissue regeneration:
How PRP Supports Erectile Function
Research indicates that PRP therapy contributes to ED recovery through multiple mechanisms:
- Promoting angiogenesis (new blood vessel formation) for improved penile blood flow
- Supporting nerve cell regeneration and myelination of axons
- Recruiting progenitor cells to damaged tissue sites
- Reducing fibrosis and protecting cells from apoptosis (cell death)
- Enhancing collagen synthesis and extracellular matrix production
- Improving smooth muscle cell content in corpus cavernosum
Stem Cell Therapy for ED
Stem cell therapy represents one of the most promising frontiers in regenerative medicine for ED. Stem cells possess the unique ability to proliferate and differentiate into specialized cell types, making them ideal candidates for repairing damaged penile tissues.
Types of Stem Cells Under Investigation
Mechanisms of Action
During the repair and regeneration process, stem cells contribute to ED recovery through several pathways:
Cellular Differentiation
Stem cells can differentiate into smooth muscle cells, vascular endothelial cells, and peripheral nerve cells to replace damaged tissue.
Paracrine Effects
Stem cells secrete exosomes, cytokines, and growth factors that promote healing in surrounding tissues without necessarily integrating into the tissue themselves.
Anti-Inflammatory and Anti-Apoptotic Activity
Stem cells help modulate immune responses and protect cells from programmed cell death, preserving tissue integrity.
Improved Nitric Oxide Signaling
Research shows increased expression of neuronal and endothelial nitric oxide synthase (nNOS and eNOS), which are essential for achieving erections.
Among stem cell sources, adipose-derived stem cells (ADSCs) have been the most extensively studied for ED. Their advantages include ease of harvesting, abundance, reduced risk of tissue rejection (when autologous), and demonstrated efficacy in preclinical models.
Low-Intensity Shockwave Therapy (LI-ESWT)
Low-intensity extracorporeal shockwave therapy has emerged as a non-invasive treatment option for vasculogenic ED. The therapy uses acoustic pressure waves that compress and then expand targeted tissues, triggering biological responses that promote healing.
Therapeutic Benefits of LI-ESWT
- Activates release of angiogenic factors to promote new blood vessel formation
- Improves blood flow and hemodynamics in penile tissue
- Increases homing of stem/progenitor cells to treatment areas
- Activates Schwann cells and releases neurotrophic factors
- Upregulates VEGF, nNOS, and alpha-smooth muscle actin (α-SMA)
- Can improve response to PDE5 inhibitors in previously non-responsive patients
Research suggests that combining LI-ESWT with other regenerative therapies, such as stem cells or PRP, may produce synergistic effects that enhance overall treatment outcomes.
The Power of Combined Therapies
One of the most exciting developments in regenerative ED treatment is the combination of multiple therapeutic approaches. Research indicates that pairing different regenerative modalities often produces better outcomes than any single treatment alone.
Key Research Finding
Studies in diabetic ED rat models demonstrated that combined adipose-derived stem cell therapy with low-intensity shockwave treatment produced superior therapeutic effects compared to either treatment administered individually. Both therapies increased expression of α-smooth muscle cells, nNOS, and Von Willebrand factor in corpus cavernosum tissue.
PRP has also been shown to enhance the effectiveness of stem cell therapies. The growth factors in PRP create a supportive environment that promotes stem cell proliferation, differentiation, and survival. This biological synergy makes combination protocols particularly promising for clinical applications.
Future Directions and Clinical Implications
Regenerative therapies represent a paradigm shift in ED treatment—moving from symptom management to actual tissue restoration. While many of these approaches are still being refined through ongoing research, several key conclusions have emerged:
- Stem cells and PRP offer safe, autologous treatment options with prolonged efficacy compared to conventional therapies
- Regenerative approaches target the underlying causes of ED rather than temporarily masking symptoms
- Combination protocols may offer enhanced outcomes through synergistic mechanisms
- These therapies show particular promise for men who have not responded to conventional treatments
- Further clinical trials are needed to establish standardized protocols and long-term outcomes
Important Consideration
While regenerative therapies show tremendous promise, they should be administered by trained medical professionals using established protocols. Patients considering these treatments should consult with qualified healthcare providers who specialize in regenerative medicine and men's sexual health.